Others
Working with the People’s Republic of China to Pilot Public-Private Partnership in Elderly Care
13 Nov 2019
ADB is working with the People’s Republic of China to pilot public-private partnership in elderly care.
How to deal with the elderly is a pressing challenge for the People’s Republic of China with the number of the over 65s set to rise from 142 million in 2016 to 289 million, or 20% of the population, by 2034.
In the People’s Republic of China, ADB is working with the local government in Yichang, a third-tier city in the Yangtze River Economic Belt region, to structure a public-private partnership that will demonstrate how the government and private entities can work together to provide better elderly care services.

Li Zheng and his wife thought that his son and daughter-in-law would look after them when they got old but since they moved away, they will have to make other arrangements.
“When I reach the age when I have physical difficulties, I will definitely want to go to an old-age residential home,” said the 84-year-old Mr. Li, a retired engineer now living in central Beijing, in the People’s Republic of China (PRC). “I think a good elderly care system should include good surroundings, good facilities for entertainment, and good food, as well as easy access to hospital and healthcare.”
“Private sector technical and operational expertise as well as possible funding will be crucial to tackling the complexities of elderly care” Hiroko Uchimura Shiroishi, Senior Social Sector Specialist, East Asia Department.
The decisions facing Mr. Li and his wife are typical in the PRC which has seen the number of its elderly soar in recent decades even as their children, who in the past would have looked after them, are moving away in search of jobs.
How to deal with the elderly is a pressing challenge for the PRC too with the number of the over 65s set to rise from 142 million in 2016 to 289 million, or 20% of the population, by 2034 (ADB Briefs, 2018). The country will have some 98 million people aged 80 years or more by then too, up from just 18 million now (ADB Project). However, other countries in the region will also need to address this issue sooner or later.
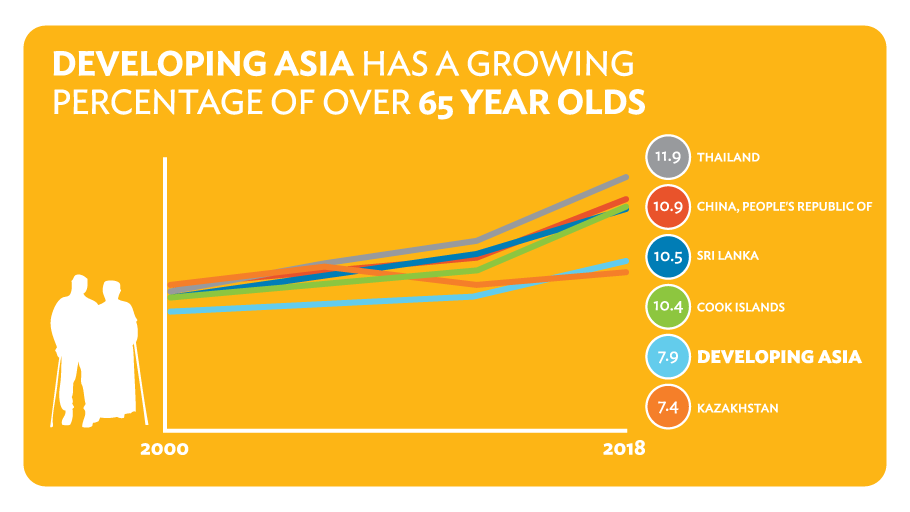
By 2018, for example, 11.9% of Thailand’s population was aged 65 years or more, up from 6.5% in 2000, but even countries still enjoying a demographic dividend such as India, the elderly now makes up a larger 6.2% of the population and 5.9% in Indonesia (Key Indicators).
“Economies will slow if the region doesn’t deal with its greying population. Asia is unique in that it is aging much faster than other regions and so it needs new solutions specific to the region,” said Donghyun Park, Principal Economist with the Asian Development Bank’s (ADB) Economic Research and Regional Cooperation Department.
Governments though face numerous calls on their finances and have little experience providing elderly care. Needs can vary with some cities aging more rapidly than others. Some elderly need intensive care to tackle dementia or physical disabilities while others may need only intermittent care at home. Elderly care also needs to be coordinated with overall healthcare.
“Private sector technical and operational expertise, as well as possible funding, will be crucial to tackling this,” said Hiroko Uchimura Shiroishi, Senior Social Sector Specialist with ADB’s East Asia Department, noting that while spending on elderly care is going up, it isn’t rising as fast as it needs to. In Asia, government assistance to the elderly in the form of noncontributory transfers or social pensions averages only 0.2% of aggregate gross domestic product, with only five countries – the Maldives, the Republic of Korea, Thailand, Mongolia, and Nepal – spending more than that (Social Protection Index).
In the PRC, ADB is working with the local government in Yichang, a third-tier city in the Yangtze River Economic Belt region, to structure a public-private partnership (PPP) that will demonstrate how the government and private entities can work together to provide better elderly care services. Under the PPP, the Yichang local government will build the elderly care facilities while the private entity will run them, providing different levels of care. An upcoming project in the southern Guangxi Zhuang Autonomous Region will build on this work to train and develop another PPP project in which the private sector partner will both build and run the elderly facilities and services.
Another PPP project in the pipeline in Xiangyang, Hubei Province will further help develop a range of care services, including residential care, daycare, rehabilitation, and geriatric medicine.
“Across developing Asia, there is a huge lack of knowledge within local governments about the intricacies of social sector PPP design, procurement, and contract management,” said Srinivas Sampath, Chief of ADB’s PPP thematic group. “Promoting a mechanism for genuine and transparent PPPs that can be replicated would allow the region to tackle the funding gap and the complex issues around elderly care.”
Services will focus around a three-tier system comprising options for elderly care in elderly residences, in the community, or from their home rather than simply building more old-age homes with more beds. This 3-pronged approach is in line with international trends which recognizes that delivering services to the elderly in their own home is both better for the older person, more cost-effective in the long-run, and allows family carers to return to the labor market.

And the projects will also help improve training for the large numbers of caregivers, nurses, physiotherapists, and others needed to ensure the elderly stay fit and healthy as long as possible.
This article is reproduced from Asian Development Bank.


